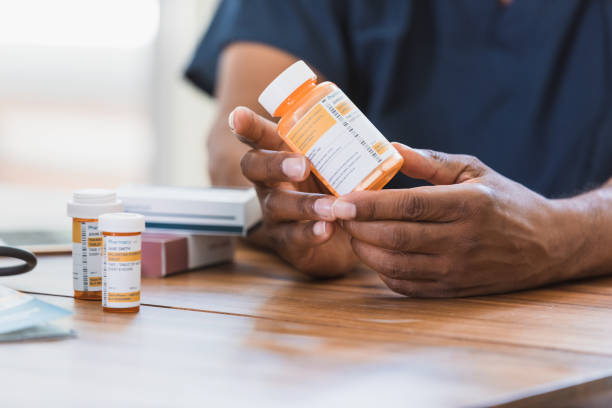
Drug interactions is the way different medications can interact with one another, either enhancing or diminishing their effects. It’s like a complex dance happening inside our bodies, where medications may interfere with each other’s intended actions, leading to unexpected outcomes.
Imagine taking a painkiller for a headache while also using an over-the-counter cold medication. Without being aware of potential drug interactions, you might unknowingly put yourself at risk for adverse effects. It’s vital to have a grasp on how different medications can potentially interact to prevent any unwanted surprises along the way.
In this blog post, we’ll dive deeper into the world of drug interactions, providing you with essential tips to ensure safe and effective medication use. So buckle up, and let’s explore this fascinating topic together!
Types of Drug Interactions
1. Pharmacodynamic Interactions
Pharmacodynamic interactions occur when two or more medications affect the same physiological pathway or target in the body, resulting in an altered response.
To give you a clearer picture, let’s consider an example. Say you’re taking medication for high blood pressure, and at the same time, you’re prescribed a muscle relaxant. Both medications work on the nervous system but in different ways. Now, if they interact pharmacodynamically, it could lead to excessive relaxation and a drop in blood pressure, potentially causing dizziness or fainting.
2. Pharmacokinetic Interactions
These interactions involve changes in the absorption, distribution, metabolism, or elimination of a drug, altering its overall concentration and effectiveness in the body.
To put it simply, imagine you’re taking a particular medication that is broken down by a specific liver enzyme. But, you also start using another medication that inhibits the activity of that same enzyme. As a result, the first medication may not be broken down properly, leading to increased levels in the bloodstream and a higher risk of side effects.
3. Combined Pharmacodynamic and Pharmacokinetic Interactions
Sometimes, the lines between pharmacodynamic and pharmacokinetic interactions blur, leading to combined interactions. In these cases, medications can both affect the same physiological pathway and interfere with each other’s absorption, metabolism, or elimination.
Let’s say you’re taking a medication for depression that also acts as a strong inhibitor of a liver enzyme responsible for metabolizing certain pain medications. This combination can result in increased levels of the pain medication in your system, leading to potential toxicity.
Factors Contributing to Drug Interactions
1. Genetics
Our genetic makeup can play a significant role in how we metabolize medications. Enzymes in our bodies, responsible for breaking down drugs, can vary from person to person based on genetic factors. This means that individuals with certain genetic variations may metabolize medications differently, potentially increasing the risk of drug interactions. Genetic testing and personalized medicine are emerging fields that aim to better understand these variations and optimize medication regimens accordingly.
2. Age
Our bodies undergo changes as we grow older, including alterations in organ function and metabolism. The elderly population tends to be more susceptible to drug interactions due to these age-related changes. It’s essential for healthcare providers to consider age-related factors when prescribing medications to older adults and closely monitor for potential interactions.
3. Gender
Gender can influence how medications are absorbed, distributed, metabolized, and eliminated in the body. Hormonal differences between males and females can impact the effectiveness and potential interactions of certain drugs. For example, hormonal contraceptives can affect the metabolism of various medications, leading to potential interactions. Recognizing these gender-related differences is crucial for healthcare providers to provide personalized care and minimize the risks of drug interactions.
4. Other Medical Conditions
Certain health conditions can affect the metabolism and clearance of drugs from the body, potentially leading to interactions. It’s important to inform your healthcare provider about any existing medical conditions so that they can make informed decisions about prescribing medications and monitor for potential interactions.
5. Medication History
Your medication history is a vital piece of the puzzle when it comes to drug interactions. The combination of multiple medications increases the risk of interactions. Additionally, previous experiences with certain medications, such as allergic reactions or adverse effects, should be taken into account when prescribing new medications. Openly discussing your medication history with your healthcare provider allows them to make informed decisions and minimize the risk of drug interactions.
6. Dietary and Herbal Supplements
Remember, it’s not just prescription and over-the-counter medications that can interact with each other. Dietary supplements and herbal remedies can also play a role in drug interactions. Certain supplements and herbs can affect the metabolism of medications or have similar effects, potentially leading to unwanted interactions. It is very important to inform your healthcare provider about any dietary supplements or herbal remedies you are taking to ensure they can assess potential interactions and provide appropriate guidance.
How to Prevent and Manage Drug Interactions
1. Communicate with your Healthcare Providers
When it comes to preventing and managing drug interactions, open communication with your healthcare providers is key. Don’t hesitate to ask questions about potential interactions when starting a new medication. They are there to help you and can provide valuable insights. Additionally, ensure you provide a complete and up-to-date list of all the medications, including over-the-counter drugs and supplements, you’re currently taking. This information will enable your healthcare provider to identify any potential interactions and make informed decisions regarding your treatment.
2. Read Labels and Instructions
Take the time to read labels and instructions on medications carefully. Look out for any warnings or precautions regarding drug interactions. Some medications may have specific instructions regarding food or other medications that should be followed to avoid interactions. By being aware of these instructions, you can minimize the risks associated with drug interactions. If you have any doubts or concerns, don’t hesitate to consult your healthcare provider or pharmacist for clarification.
3. Use a Medication Management System
Consider using a medication management system to help you stay organized. These can range from simple pill organizers to smartphone applications. By using such tools, you can ensure you take the right medications at the right times and avoid potential interactions. Some systems even allow you to set reminders for dosage and administration, helping you stay on top of your medication regimen.
Here are some tools you can use:
- The Medisafe App
- Mango Health
- Bedsider Reminders
Conclusion
We’ve explored different types of interactions, contributing factors, and practical tips. By communicating with healthcare providers, reading labels, and using medication management systems, you can minimize risks and ensure your well-being. Prioritize open communication, follow instructions, and stay organized.
With these practices, you’re taking control of your health journey and creating a safer medication experience. Here’s to informed decisions, optimal health, and a life free from drug interaction risks. Stay well, and take care!
Research links:
https://www.fda.gov/drugs/resources-you-drugs/drug-interactions-what-you-should-know
https://www.nps.org.au/consumers/understanding-drug-interactions
https://avilahomecare.com/news/2019/11/medication-management-how-avila-can-help
https://medssafety.com/what-is-drug-interaction
AUTHOR’S BIO:
Teniola Adedeji is a licensed pharmacist and CEO/founder of Pharmarun, a healthcare company that operates at the intersection of business and healthcare. With over 10 years of experience in the pharmacy and healthcare industry, Teniola has worked at various levels of the industry, including chain pharmacies like Medplus and key regulators in Nigeria like NAFDAC. Teniola’s experience also extends to investment banking, where she worked with Bank of America Merrill Lynch and Goldman Sachs Asset Management, advising healthcare, biotech, and pharmaceutical corporations across Europe, the Middle East, and Africa. With her deep understanding of the healthcare industry’s inner workings and her expertise in investment banking, Teniola is committed to driving innovation in the healthcare industry. To learn more about Teniola, click here https://www.linkedin.com/in/teniola-adedeji-526b0880/
Website Link: www.pharmarun.africa
YOU SHOULD ALSO READ:
- List of Items Required During Delivery in Nigeria
- The Basic Items In A First Aid Box in Nigeria
- 103 Medical Abbreviations in Nigeria and their Full Meaning
- 7 Drugs To Have At Home In Nigeria
- 5 Ways To Be Eco-Friendly in Nigeria
- 5 Things To Consider Before Getting Health Insurance In Nigeria
- 5 Common Drugs Banned In Nigeria
Collins Nwokolo is a human physiologist, writer and health enthusiast. He loves writing helpful articles on health and fitness, which he enjoys sharing with everyone.